Merkel carcinoma
Everything to know about Merkel carcinoma
Merkel cell carcinoma is the eponymous name for primary cutaneous neuroendocrine carcinoma. Merkel cells are normal cells found in the epidermis (the outer layer of the skin). These cells function primarily as mechanoreceptors and produce certain hormones. Merkel cell carcinoma results from uncontrolled proliferation in the skin of cells that share some characteristics with normal Merkel cells.
The main risk factors are UV radiation exposure, immunosuppression, and clonal integration of the Merkel cell polyomavirus.
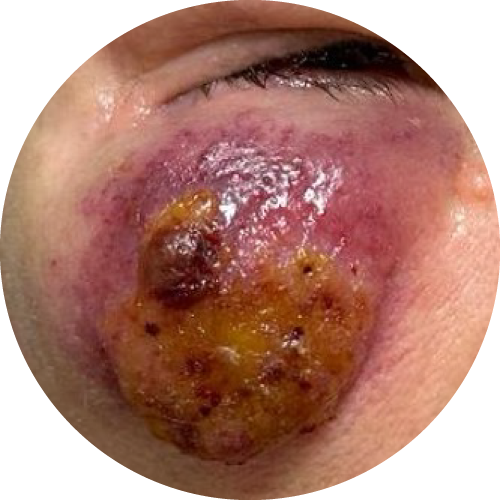

Merkel cell carcinoma usually presents as a skin-colored or violaceous nodule or plaque with rapid growth. It tends to progress quickly without causing pain or hypoesthesia.
Surgery is the reference treatment for Merkel cell carcinoma. It should be performed urgently, either under local or general anesthesia depending on the complexity and duration of the procedure, and is combined with sentinel lymph node biopsy. Given the aggressiveness of this tumor, wide resection margins are recommended to ensure complete removal. Reconstruction is performed during the same operation and often requires flaps and grafts. In many cases, a lymph node dissection is required, as well as adjuvant radiotherapy. In all cases, a multidisciplinary tumor board (MDTB) discussion is held to determine the optimal management strategy, based on tumor aggressiveness, stage, and surgical results.
Immunotherapy may also be offered in cases of metastatic disease, and numerous studies are underway to better define its role.
Merkel cell carcinoma is a highly aggressive tumor with a risk of lymphatic metastasis. In addition to regular clinical follow-up, further staging with head and neck imaging (ultrasound, CT scan) and whole-body imaging (18F-FDG PET scan) in cases of lymph node involvement should be performed during follow-up, after an initial preoperative staging evaluation to assess tumor dissemination.